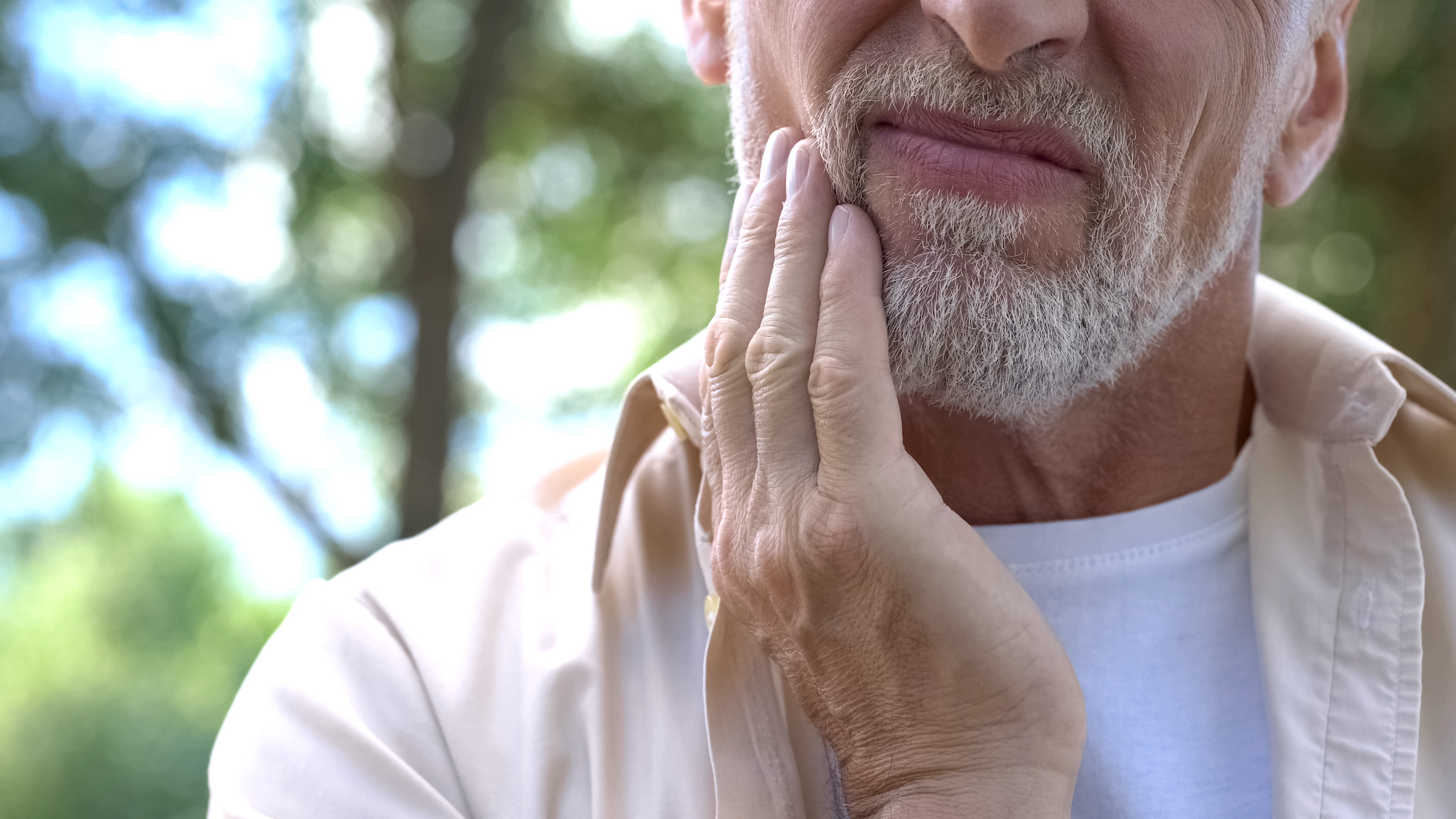
Towering costs are having a detrimental impact on New Zealanders unable to afford dental healthcare.

The poor state of dental health in New Zealand has been highlighted in a new report Tooth be told commissioned by the Association of Salaried Medical Specialists (ASMS) and supported by Auckland City Mission – Te Tāpui Atawhai.
The report found 40 per cent of New Zealanders – and half of Māori and Pasifika people – can’t afford dental care. In 2020, it found New Zealand recorded the highest unmet need for adult dental care among 11 comparable countries.
In January, Stats NZ reported the consumer price index increased 7.2 per cent in the 12 months to December 2022.
There has been a 30 per cent rise in the number of people who need hospital-level dental care – which happens when problems are left too long, it states. In fact, the situation is so bad that the country has stopped reporting some figures internationally.
“Universal dental care is critical to the good health of everyone in Aotearoa with cost benefit analysis showing every dollar invested in dental care will return $1.60 to the country. Despite this, no government has developed or implemented a plan to provide it,” ASMS chief executive Sarah Dalton said.
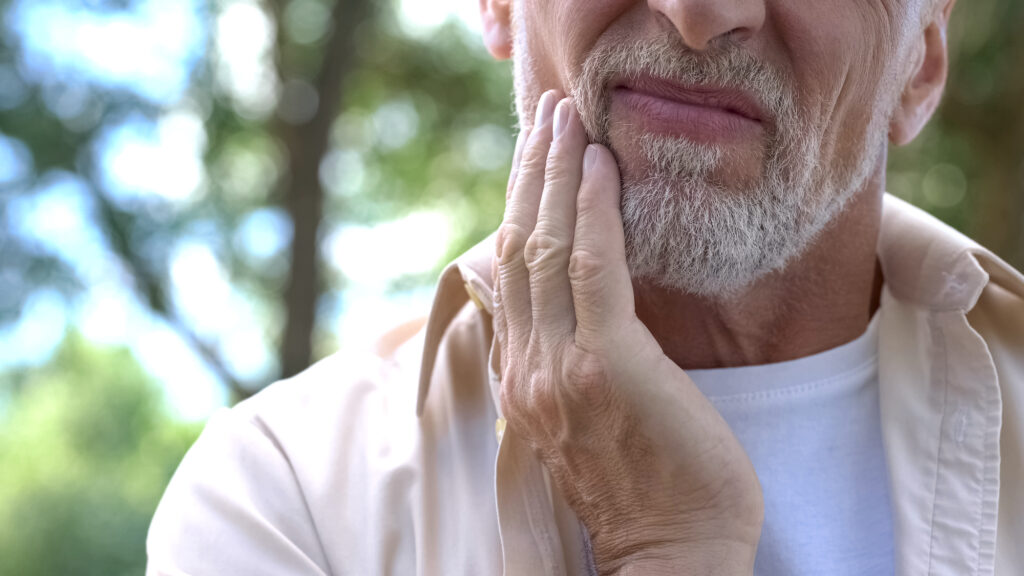
Auckland City Mission – Te Tāpui Atawhai missioner Manutaki Helen Robinson said when circumstances prevent someone from practising daily oral habits, or they can’t afford dental care, it was easy to suffer poor dental health.
While a wide range of ages have been impacted across the board, for New Zealand’s elderly community, healthcare in general is a big issue.
With more than 60 per cent of Kiwis aged over 75 suffering from gum disease and more than one in three having complete tooth loss, a shortage of sufficient oral healthcare for older individuals is having serious implications on their health and wellbeing.
Those in residential aged care facilities (RACF), experience the poorest oral health in New Zealand, with 21.8 per cent of people aged over 65 years having untreated dental decay and 53.4 per cent with periodontal disease (gum disease).
This high prevalence of poor oral health is concerning due its associated links with coronary heart disease, cognitive decline, malnutrition, diabetes and respiratory conditions such as aspiration pneumonia. Furthermore, poor oral health plays a significant role in diminished quality of life, appearance, self‐esteem and confidence of older people.
Age Concern’s chief executive Karen Billings-Jensen said: “One of the biggest concerns is that poor teeth or poor dentures can actually have a huge impact on healthy eating and even the ability to get the good foods that help keep us healthy.”
Billings-Jensen said for some older people travel can be a barrier on top of cost, and while she acknowledges there are some discounts for SuperGold or Community Services Card holders, expense is still a barrier.
She said the longer communities go without seeking dental healthcare help, the more destructive it can be to their overall health.

Should free dental healthcare be pushed as an election issue?
Before former prime minister Jacinda Ardern announced her resignation, she stated that while everyone would love free dental healthcare in principle, it was prohibitively expensive. In a 2020 report, the Ministry of Health estimated that the cost of extending free dental care to adults would tally up to $648 million per annum.
The New Zealand Dental Association proposed a stepwise approach to target the most in need first, and this finally came into fruition during Budget 2022 – with dental grants for low-income families increased from $300 to $1000.
This was the first increase since the early 90s, and the next funding increase has been proposed for 18 to 24-year-old low-income adults.
The Senior Dentists Union continues to call for free universal dental care, but as to whether it should be an election issue is a difficult question to answer – most agree however, it could do with more Government intervention and improvement.
The majority believe that in an ideal world free dental healthcare would be “fantastic”, but even having it partially funded for more New Zealanders would be a step forward, but Billings-Jensen said the issue needs to be looked at broadly, and a subsidy isn’t the only answer.
“We know access to good oral health care would make an enormously positive difference to the overall health of people we support and many others who suffer the indignity of poor oral health. It truly is a basic human right and need to be committed to helping people access that right.”
Excerpts of this article first appeared in NZ Herald